Case Studies
Case Histories from the Bayside Breastfeeding Clinic
Names and some details have been changed to protect privacy.

Unable to Tolerate Solids Until AfterTwelve Months
Unable to Tolerate Solids Until After Twelve Months ‘Cindy’ was concerned that any attempt to give solids to eight month old ‘Peter’ was an utter disaster. Every time he had
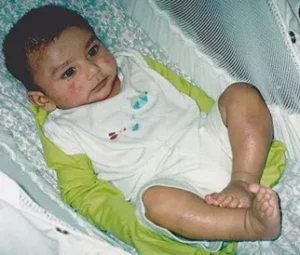
Resolving eczema in a fully breastfed baby
Resolving eczema in a fully breastfed baby Despite often being covered in weeping, itching eczema, four month old ‘Kevin’ was usually a surprisingly happy baby. His mother ‘Roxy’ had cleverly
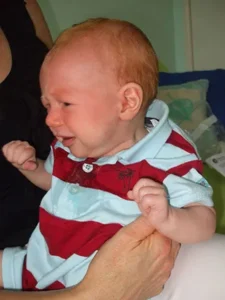
Constant Vomiting and Unhappiness in a Fully Breastfed Baby
‘Jenny’ described three months old ‘Thomas’ as her ‘velcro baby’ because she couldn’t put him down without him ‘crying pitifully, as if he’s been abandoned’. Thomas spent a lot of
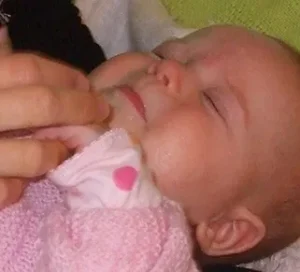
Breast Refusal Due to Maternal Diet
Breast Refusal Due to Maternal Diet Aged five months, baby ‘Krystal’ had changed dramatically from the peaceful breastfeeder she had been up until about eight weeks old. Things had become
